Connect With Us
Blog
Items filtered by date: July 2021
What Does Uric Acid Have to Do with Gout?
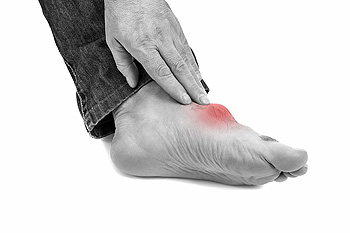
Uric acid is a byproduct of the process your body goes through as it breaks down purines, chemical compounds that naturally occur in your body as well as in certain foods such as red meat, seafood and alcoholic beverages. Normally, most uric acid is reabsorbed back into the body, or expelled through the kidneys. When your body produces too much uric acid (or has difficulty flushing it), hard, crystal-like deposits build up in and around the joints. This is known as gout. While this painful condition may manifest in any joint of the body, it most commonly occurs in the metatarsophalangeal joint of the big toe. These sharp urate crystals can cause severe flare-ups of pain, swelling, tenderness and heat in the affected joint. Symptoms tend to develop quickly and occur more often at night. They can come back and increase in frequency if the underlying condition is not treated properly. Contact a podiatrist for an exam, and to discuss possible treatments for this painful arthritic condition.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact Dr. John R. Northrup from Superior Foot, Ankle & Wound Care. Our doctors will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions please feel free to contact one of our offices located in St. Augustine, and Palm Coast, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Does It Hurt to Freeze a Foot Wart?
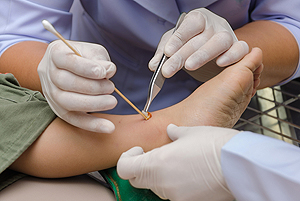
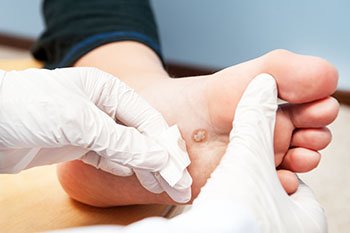 Plantar warts, which grow on the bottom of the feet, can be removed by freezing them off in a treatment called cryotherapy. During this procedure, the doctor cuts the wart with a small, sharp knife and then applies a freezing substance, such as liquid nitrogen, with a cotton swab or spray. Cryotherapy can hurt, and your doctor may use a local anesthetic to reduce pain. The treatment itself takes only a few minutes. Following the procedure, your foot may hurt for two to three days. A blister can form over the site of the wart but will typically disappear within a few days. There is a chance for minimal scarring. If you have a wart on the bottom of your foot, it is suggested that you consult a podiatrist to see if cryotherapy is the right treatment for you.
Plantar warts, which grow on the bottom of the feet, can be removed by freezing them off in a treatment called cryotherapy. During this procedure, the doctor cuts the wart with a small, sharp knife and then applies a freezing substance, such as liquid nitrogen, with a cotton swab or spray. Cryotherapy can hurt, and your doctor may use a local anesthetic to reduce pain. The treatment itself takes only a few minutes. Following the procedure, your foot may hurt for two to three days. A blister can form over the site of the wart but will typically disappear within a few days. There is a chance for minimal scarring. If you have a wart on the bottom of your foot, it is suggested that you consult a podiatrist to see if cryotherapy is the right treatment for you.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Dr. John R. Northrup from Superior Foot, Ankle & Wound Care. Our doctors will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact one of our offices located in St. Augustine, and Palm Coast, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The Wagner Diabetic Foot Ulcer Classification System
If you suffer from diabetes, you may be familiar with the increased risk of developing poorly healing wounds on your feet. Small cuts, sores, or scrapes can go unnoticed due to neuropathy or nerve damage, and heal slowly because of poor circulation. These issues can make wounds grow larger and become infected, turning into diabetic foot ulcers (DFUs). There are various classification systems for describing the general characteristics of these wounds. Doctors who use the Wagner system classify DFUs by their severity, in a graded system ranging from 0 to 5. A Grade 0 ulcer means that the skin is intact. Grade 1 signifies a superficial ulcer on the outer layers of skin. Grade 2 is a deep ulcer. Grade 3 is an ulcer with bone involvement. Grade 4 means that there is gangrene or dead tissue in the front of the foot, while Grade 5 means that the gangrene has spread to the entire foot. If you notice any wounds on your feet, please schedule an appointment with a podiatrist who can treat wounds and help you manage your condition.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dr. John R. Northrup from Superior Foot, Ankle & Wound Care. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact one of our offices located in St. Augustine, and Palm Coast, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Arthritis Can Cause Pain in the Feet and Ankles
The Three Stages of an Ingrown Toenail
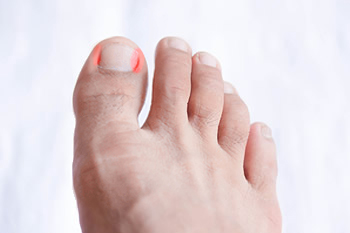
Ingrown toenails occur when the edge of a nail grows into the surrounding skin rather than over it. An ingrown toenail can be classified into one of three categories based on its severity. A Stage 1 ingrown toenail is characterized by the end of the toe becoming red and mildly swollen, warm, or painful to the touch, but with no pus or drainage. A Stage 2 ingrown toenail is characterized by increased redness, swelling, and pain, white or yellow-colored pus or drainage from the area, and infection. A Stage 3 ingrown toenail will usually have even more severe redness and swelling, be very painful, and be accompanied by an overgrowth of skin around the toenail. More severe infection and a fever may follow. If you frequently experience ingrown toenails, or if your toenail is showing signs of infection, it is suggested that you seek the care of a podiatrist as soon as possible.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact Dr. John R. Northrup of Superior Foot, Ankle & Wound Care. Our doctors can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact one of our offices located in St. Augustine, and Palm Coast, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.